Peutz Jeghers Syndrome
What is Peutz jeghers Syndrome?
Peutz jeghers syndrome is an inherited genetic disorder causes abnormality in mutation and outcome can be noncancerous multiple polyps formation or hamartomas in the mucous membrane of the gastrointestinal tract, specifically in intestine and stomach.
The presence of Peutz jeghers syndrome increases cancer development almost 15-fold more than the normal individual. Often Peutz jeghers syndrome turns to cancerous tumor formed in breast, gastrointestinal tract, pancreas, cervix and ovary.(1,2)

Signs & Symptoms
Peutz-jeghers syndrome has following sign and syndrome:
Discolor spot in skin
After development of the peutz-jeghers syndrome, dark skin discoloration is a definite symptom of the affected person. The usual affected body parts are surrounding area of the eye, lips, nostrils, inside the oral cavity, mucous layer in the mouth and perianal area, inside the mouth and in the finger.
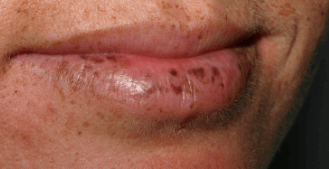
This symptom is developed due to added melanin deposition. The hyperpigmentation of childhood may lighten with increase of age.
Polyps in GIT
Multiple benign polyps or tumors present in the mucous membrane of the gastrointestinal system. These benign polyps are termed as hamartomas. The usual affected site is the small intestine, but stomach and large intestine also may involve. This sign characteristically provides the following symptoms:
- Chronic rectal bleeding
- Anemia
- Bowel collapse or obstruction
Females
Hormonal abnormality is common in females due to the presence of peutz-jeghers syndrome. Often the peutz-jeghers syndrome causes benign tumor formation in the ovary called sex cord tumors with annular tumors (SCTAT). This may associated with early onset of puberty, irregular menstrual cycle or heavy bleeding during periods.
Males
If peutz-jeghers syndrome is develop in males, then tumor may develop in the testis, which secretes estrogen. This can lead to gynecomastia or breast development. (1,2,4)
Causes
Peutz-jeghers syndrome is an autosomal dominant hereditary disorder. Abnormal genetic mutation is the cause of the development of the Peutz-jeghers syndrome.
Abnormal mutation in the STK11 gene is associated with Peutz-jeghers syndrome. In normal human, STK11 gene is responsible for tumor suppression, means it prevents the excessive, uncontrolled or abnormal growth of the cells.
But due to abnormal mutation, the structural or functional disorder develops in the STK11 protein, which causes an interruption of its capability to hold back unnecessary cell proliferation.
The consequential abnormal cell division leads to the development of the noncancerous polyps, which usually turns to cancerous tumors of the affected individual with Peutz-Jeghers syndrome.
The individual affected with inherited Peutz-Jeghers syndrome has an autosomal dominant pattern of genetic abnormality. This means, single copy of the distorted gene in every cell is enough to augment the possibility of progressing hamartomas and then they turn to cancerous tumors.
Almost 50% cases of Peutz-Jeghers syndrome have the tendency of involvement of the inherited abnormal mutation in the STK11 gene from either affected mother or father, though the other cases do not have a family history of Peutz-Jeghers syndrome. These cases may arise due to consequence of de novo (new) mutations in the STK11gene.
But in rare cases, the abnormal STK11 gene mutation does not involve in the formation of polyps in the Peutz-Jeghers syndrome. The cause of development of those cases are yet unknown. (4,5)
Diagnosis
A symptomatic diagnosis means the presence of polyps in the small intestine is the prime finding of Peutz-Jeghers syndrome. Usually gastrointestinal related symptoms of Peutz-Jeghers syndrome are diagnosed at the age of 10years of an affected child.
Genetic council and latter for confirmation genetic testing is needed to detect the affected person. For genetic testing blood sample is collected for checking the STK11 gene mutation, if the test result is positive, then same test is conducted with other family members and tested the same gene mutation. However, in some cases, affected individual may not have a detectable mutation in STK11. (3,4)
Treatment
Routine follow-up of small intestinal polyps can prevent intestinal impediment and progression to cancer. An imaging technique like endoscopy is conducted for overseeing the internal membranous structure of the intestine helps to detect the presence of larger sized polyp (>1 cm) and that should be needed to remove during the procedure.
Screening for cancer is conducted depends upon the family history and the test result obtain from the regular examination.
Females with PJS, often reported with breast cancer, so the clinical breast examination and mammography are important to evaluate after 20 years of age for detecting the early onset.
A testicular examination should regularly perform in men with PJS. The affected individual with other family members need genetic counseling. (4)
Life Expectancy
The risk of gastrointestinal cancer is higher in individuals with Peutz-Jeghers syndrome than normal individuals. The Peutz-Jeghers syndrome with cancer progression causes 48% of death within the age of 57 years. If cancer is not developed then affected individual may have a normal life span. The most of the identified data supports that onset of cancer is more common in the age of 42.9 years, ±10.2 years. (1)
Images
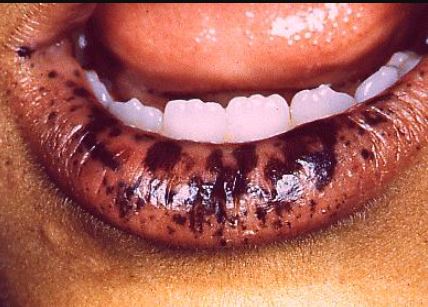
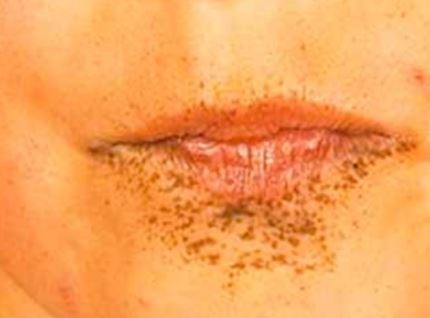
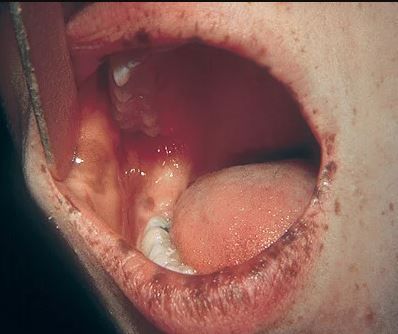
References
- Thomas M Attard (2015); Peutz-Jeghers Syndrome; http://emedicine.medscape.com/article/182006-overview
- Genetic Home Reference (2013); Peutz-Jeghers syndrome; https://ghr.nlm.nih.gov/condition/peutz-jeghers-syndrome
- Peutz-Jeghers Syndrome (2014);cancer.Net Editorial Board; http://www.cancer.net/cancer-types/peutz-jeghers-syndrome
- Peutz Jeghers Syndrome (2007); National Organization for Rare Disorders; http://rarediseases.org/rare-diseases/peutz-jeghers-syndrome/
- Peutz-Jeghers syndrome; DermNet NZ; http://www.dermnetnz.org/systemic/peutz-jeghers.html
- Kristin Zelley (2012); Peutz-Jeghers Syndrome (PJS); http://www.chop.edu/conditions-diseases/peutz-jeghers-syndrome-pjs#.VtuShVt97IU
