Pilon Fracture
What is Pilon Fracture?
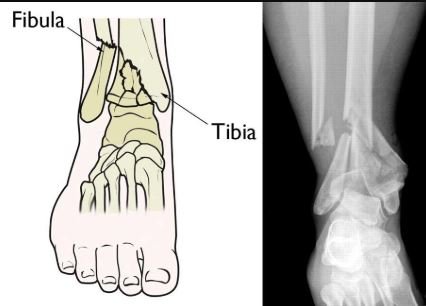
Your lower leg has two bones called tibia and fibula. Pilon fracture refers to the injuries that affect the lower end of your tibia and the surface that bears weight of ankle joint. These injuries can also damage your fibula. You can experience various pilon fractures such as:
- Your tibia can break in one place of the leg, or
- It can split into many pieces.
The lower leg has two bones which are tibia, also known as shinbone, and fibula, a small bone. There is also the talus part, which is a small bone of the lower leg that acts like a hinge between fibula and tibia. The ankle joint is made up of these three bones (talus, fibula, and tibia)
The acuteness of pilon fractures in individuals may depend on several factors such as:
- How many fractures do you have?
- The number and the size of broken bone ligament
- The number of bones displaced
- The damage to the nearby soft tissues such as skin, muscles, ligaments, and tendons.
If the damage causes the bone to break and the bone fragments penetrate through your skin, the fracture is referred to as open or compound fracture. This form of fracture is very severe because you are vulnerable to various infections in the bone and skin when the skin is broken.
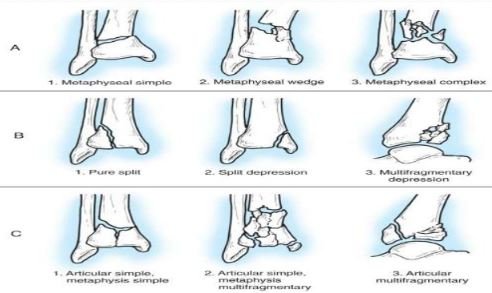
Pilon Fracture Types
Causes
You can get a pilon fracture when you are involved in high-energy activities and injuries such as accidents from a motorcycle and skiing accidents. When you fall from a high building or tree, you may also experience a pilon fracture.
Symptoms
Individuals with a pilon fracture can have the following symptoms:
- You feel pain and inability to tolerate the load on the leg
- Pilon fracture can also cause deformity of your ankle joint
- There is visible swelling on your leg and bruising.
Diagnosis
A pilon fracture can be diagnosed using various methods such as:
Physical examination
The first step requires a physical examination of your leg and ankle. Your doctor or surgeon determines your medical history including the symptoms, medicine used, and diseases and conditions you suffered from in the past. Your doctor then performs a physical assessment in the following ways:
- Checks your ankle and lower leg to find out any cuts or injury. The doctor can gently push your lower leg and ankle to see if this hurts you or not.
- Looks for swelling in your ankle and foot
- Examines the rest of your body to find out any injuries
- Assesses whether you are able to move your toes and how you feel.
Your doctor can conduct other tests to find out the extent of a pilon fracture and the damage it has caused to your leg and ankle joint. The following imaging tests are used:
X-rays
Your surgeon or doctor will use X-rays to produce dense images of your ankle, bone, and leg. This will help your doctor determine if you have a bone injury and if any of your joint ankle bones are displaced.
Computed tomography (CT) scans
Computed tomography (CT) scans show fracture lines in your foot and ankle very clearly. This can help your doctor determine the acuteness of your facture and plan for the best treatment options.
Treatment
After diagnosis, your doctor may recommend surgery depending on the extent of your bone fracture. If your bones are minimally displaced, your doctor will treat the fracture using non-surgical interventions.
Non-surgical treatments are as follows:
Splints and Casts
Splints and casts are solid material wraps used to support and protect damaged ligaments, bones, tendons and other tissues. They can also lessen swelling and pain as well as protect the damaged site from further harm.
Splints Vs Casts
Casts are made from either plaster or fiberglass and customized for different needs. A cast covers the whole area of an injury and can only be put and removed by the doctor.
A splint comes in various shapes and sizes and can be used for different injuries. A splint does not cover the whole injured site as casts do and splints require a supportive material to maintain them in place. You can easily adjust or remove a splint unlike the casts.
Your doctor will use a splint to hold your ankle in place. As soon as swelling reduces, your doctor will replace the splint with a short leg cast. The casts will provide support to your foot and facilitates faster healing. Your doctor will also change casts as the swelling continues to reduce because a well- fitting cast provides effective support.
Checkups
Your doctor will schedule your checkups sessions. The doctor will conduct X-ray checkups during these sessions to ensure that your ankle remains stable.
Things to Avoid when you Have Cast & Splint
If a cast or splint has been placed on your ankle, you may want to refrain from the following:
- Do not put sand inside the splint or cast because they may damage your skin
- Do not use deodorants inside a cast if you experience acute itching, but instead consult your doctor
- Monitor the cast and exposed skin daily, if you observe any injury, inform your doctor
- Never use home tools to remove the cast; they will damage blood vessels.
Surgical treatment
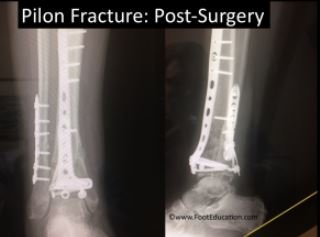
Open reduction and internal fixation
An open reduction internal fixation is a surgical procedure used to realign the bones in the normal position. Internal fixation refers to materials that keep the bone stable such as screw and plate. 2
The procedure is done to maintain the bone fracture stable in order to heal properly and prevent infections. In this procedure, your doctor will reposition the displaced bone fragment into its usual place. Then, he or she holds these displaced bones together with a screw and fixes a metal plate on the outer surface of the bone.
External fixation
This is a procedure done to immobilize your bones to enable the fracture heal faster. In this method, before your doctor makes incision into your skin. Your doctor will assess the severity of your skin damage. If your skin is seriously damaged, making the incision will damage your skin further and lead to infections. 3
If you have a damaged fibula, your doctor will conduct surgery to treat the fibula fracture first and reposition your ankle in the right place. Then your doctor will use an external fixator to grip your pilon fracture in position.
Timing surgery
The doctor may consider delaying surgery to repair the pilon facture is he or she feels that the swelling it too intense. The delay is intended to allow the swelling to reduce. Performing a surgery when the ankle is swollen could increase the risk of having an infection or complications with the incision.
After Surgery
Your doctor will help you recover quickly in the following ways:
- Prescribe pain killers to reduce pain
- Prescribe blood thinner or anticoagulant to reduce your chances of developing a blood clot.
- Conduct special exercises to improve your ankle motions.
Complications
You are likely to experience some complications, but the doctor will minimize the chances of developing such complications.
- Have damage to your blood vessels and nerves.
Reference List
- Pilon Fractures of the Ankle. http://orthoinfo.aaos.org/topic.cfm?topic=A00527
- Open Reduction Internal Fixation surgery. http://www.orthopaedics.com.sg/treatments/screw-fixation
- External fixation: Fractures and broken bone. https://www.verywell.com/external-fixation-2548519
- Pilon Fracture. http://www.aofas.org/footcaremd/conditions/ailments-of-the-ankle/Pages/Pilon-Fracture.aspx
- http://emedicine.medscape.com/article/1233429-overview
- Pilon Fractures Treatment & Management http://emedicine.medscape.com/article/1233429-treatment
