Onychomycosis
What is Onychomycosis?
Onychomycosis is a fungal infection of the toe nails or finger nails, which is considered as the most common nail disorder. It also referred to as dermatophytic oncomycosis, onycomycosis or tinea unguium that accounts about half of nail abnormalities among individuals. This may begin as a simple cosmetic concern, until it develops as a problem if left unattended.
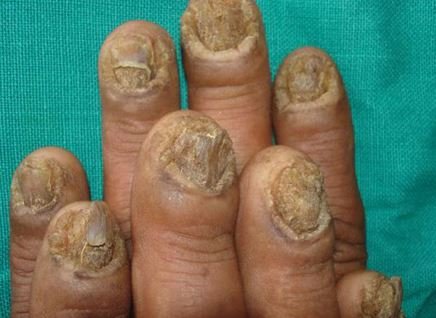
The fingernails or toenails appear thickened, discolored, disfigured and split making it not good in appearance during assessment. The thick nails can press against the inside portion of any closed-designed footwear, resulting to discomforts like pressure, irritation and pain.
This fingernail infection affects people in their psychological, social and employment standing at worksites. It usually affects adult toenails than finger nails. Increasing incidence of the condition is closely associated to patients with diabetes mellitus, suppressed immune system and with the elderly.
Symptoms
The most common sign of fungal nail infections is the thickening of the nails and its discoloration into white, black, yellow or green. The nails become brittle and splitting off as the infection progresses. Inflammation can develop and pain felt on the skin if it is not treated accordingly.
The person can be having the discomfort in walking, standing, exercising and basically all activities of daily living are at stake of not being done competently with the irritation on the site. Psychosocial concerns may arise in cases where toenails or fingers are seen publicly by others.
Types of Onychomycosis
- Distal subungual onychomycosis is the most common, affecting the nail bed and the underside of the nail plate; onycholysis can be seen which is yellowish-white in color.
- White superficial onychomycosis affects the superficial layers of the nail plates, resulting into white islands; this is confined to toenails and with white powdery patches on the surface of the nail plate.
- Proximal subungual onychomycosis affects nails of healthy people on their newly formed nail plate; the fungus attacks the cuticles of those who are immune suppressed, leukonychia develops with an inflammation.
- Endonyx onychomycosis, the fungi attacks direct the nail plate; this produces milky-white discoloration in the nail plate.
- Candida onychomycosis affects those who usually do hand immersion in water; several or all finger digits are affected, it takes a drumstick appearance.
Causes
There are three classes of fungi that may cause Onychomycosis. These are the dermatophytes, Candida yeasts and the nondermatophytes molds. Dermatophytes are the most common leading cause of Onychomycosis where Tricuphyton rubrum and Tricophyton mentagrophytes are mainly responsible.
Nondermatophyte molds such as Fusarium species and Aspergillus species are becoming more common causes worldwide. The candida yeasts are the rare cases.
The risk factors of Onychomycosis include history in the family, increasing age, poor health and nutrition, prior trauma with any types of onychomycosis, climate that is very warm or moist, several fitness activities attended, immunosuppression cases if individuals, barefooted in damp public areas, Athlete’s foot, minor skin or nail injury, common bathing places for public use; and tightly fitted shoes and wearing of socks with improper ventilation.
Aging is the most common risk factor due to weakened blood circulation, chances of prolonged exposure to fungi, and slowly growing thickened nails that predispose them to infection.
Diagnosis
There are three main approaches used to properly and correctly diagnose the occurrence of Onychomycosis among patients. These are through potassium hydrochloride smear, culture and histology.
These involves the performance of microscopic examinations and culture tests with nail scrapings or clippings and sent to laboratory for analysis to confirm the diagnosis before proceeding with specific treatment plan.
Treatment
The treatment plan depends on the specific type of onychomycosis that the patient has. Proximal subungual onychomycosis and distal subungual onychomycosis that involve the lunula region must have a long term treatment to eradicate such a discomfort.
Topical agents are being used for White superficial onychomycosis and distal subungual onychomycosis with limitation to the distal nail.
Topical antifungals are advised to patients who cannot tolerate the use of systemic treatment approach for the problem. Examples are Ciclopirox olamine 8% and Efinaconazole 10% nail solutions.
Onychomycosis is not cured by the application of topical treatments only because of the lack of nail penetration; examples are Ciclopirox and Amorolfine solutions which have been proven to penetrate through all nail layers but have lesser efficacy when used alone, they can work well together with oral medications prescribed.
Oral therapy includes the prescription of Itraconazole and Terbinafine as new medications used to treat onychomycosis. They have higher cure rates, shorter period of treatment and have fewer adverse reactions.
There are a lot of surgical approaches to onychomycosis treatment which include mechanical, chemical, or surgical nail avulsion. Urea compound with a concentration of 40-50% is used for the painless chemical removal of onychomycosis in patients.
There are instances wherein the removal of the nail plate is taken into consideration as an adjunctive treatment in patients having an oral therapy. The combination treatment approach of oral, topical, and surgical therapy can increase efficacy and reduce cost in the medical care given towards resolving all types of onychomycosis to patients.
Pictures
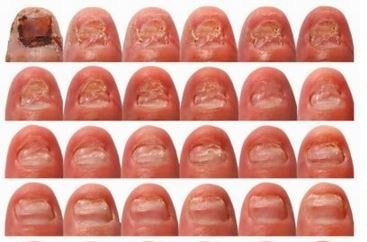
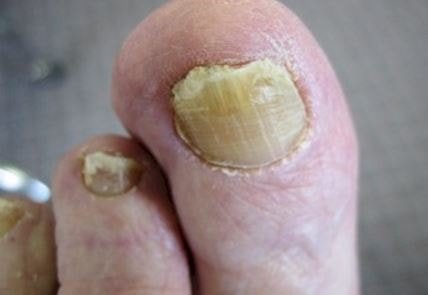
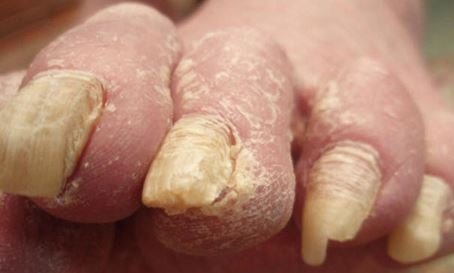
References
- http://emedicine.medscape.com/article/1105828-overview#a1
- http://www.merckmanuals.com/professional/dermatologic-disorders/nail-disorders/onychomycosis
- http://www.emedicinehealth.com/onychomycosis/article_em.htm
- Westerberg DP, Voyack MJ (Dec 1, 2013). “Onychomycosis: current trends in diagnosis and treatment.”. American family physician 88 (11): 762–70.
- Szepietowski JC, Reich A (September 2008). “Stigmatisation in onychomycosis patients: a population-based study”. Mycoses 52 (4): 343–9.
- Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. p. 1135.
