NeuroCardiogenic Syncope
What is neurocardiogenic syncope?
Medically syncope means fainting, and one of the most common findings in clinical practice. The frequent identified reasons of syncope are cardiac arrhythmia or uneven heart rate and syndromes occur due to cardio-neurological problems like neurocardiogenic syncope, which include vasovagal problem, vasodepressor.
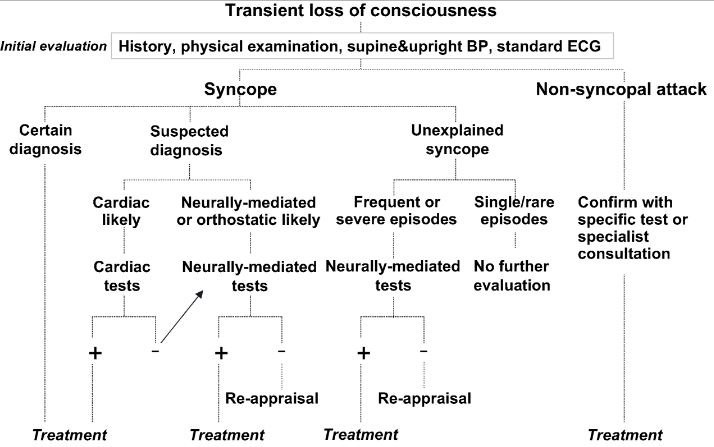
Syncopal and Non-syncopal origins of consiousness loss
Both these conditions are associated with impaired blood circulation in the brain, which causes temporary loss of consciousness.
In case of cardiac arrhythmia, tachycardia or increase heart rate has more contribution towards cause of syncope rather than bradycardia or decreased heart rate.
Neurocardiogenic syncope is also termed as “neurally mediated hypotension”. It has other clinical terms also, which include “autonomic dysfunction” “the fainting reflex”, “vasodepressor syncope” and “vasovagal syncope”. The vesovegal nerve is responsible for maintaining the blood pressure.
If the peripheral blood vessels become dilated, then blood is pooled from lower limbs and insufficient blood is reached in the brain and cause syncope or fainting.
Symptoms
Individuals who are frequently faced the neurocardiogenic syncope, the noticeable range of symptoms are observed, which include:
- fatigue
- persistent dizziness
- light headedness
- palpitation
- sudden sweating
- nausea
- muscle ache
- joint pain
- abrupt fainting
It is not necessary that all the symptoms are prominent to every individual, but abrupt fainting is common for all. Usually fatigue is a quite a problematic symptom, as it interferes with daily activities.
Even some individual has a problem with concentration, because the peripheral blood vessels are dilated and to meet the maintaining the proper blood pressure, more blood is pooled from the lower extremities. This hampers the proper circulation in the brain and mental task is constricted.
The above mentioned symptoms can further divided into pre and post fainting symptoms.
Pre fainting symptoms include:
- Skin pallor
- Tunnel vision means narrow vision, which can explain as the individual can see only the nearer objects.
- Lightheadedness
- Warm feeling
- Sweating
- yawning
- nausea
- Blurred vision
- Sudden blackout
During neurocardiogenic syncope, may the following symptoms are prominent:
- Shuddering movement
- Pulse rate become lowered down
- pupil become dilated.
The duration of fainting last only for a few seconds, but without taking a rest or abrupt postural change (lying down position to standing position) can cause the repeated fainting. It is advisable at least 15 to 30 minutes rest is essential after syncope attack.
Causes
The exact cause of neurocardiogenic syncope is unknown yet, but it is suspected that genetic reason may have the interference with this condition. This correlation is drawn, as the family history is very common findings.
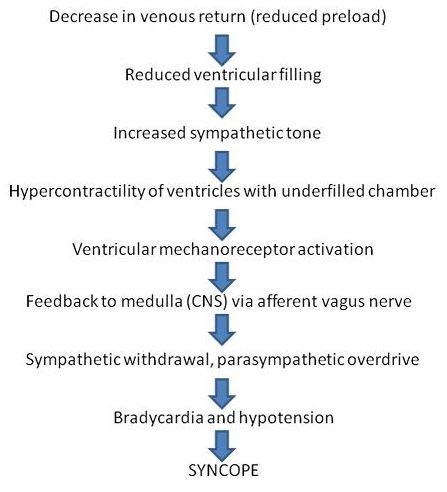
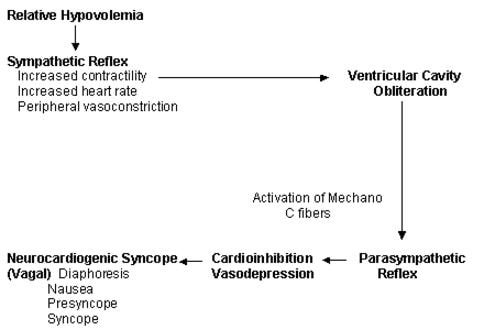
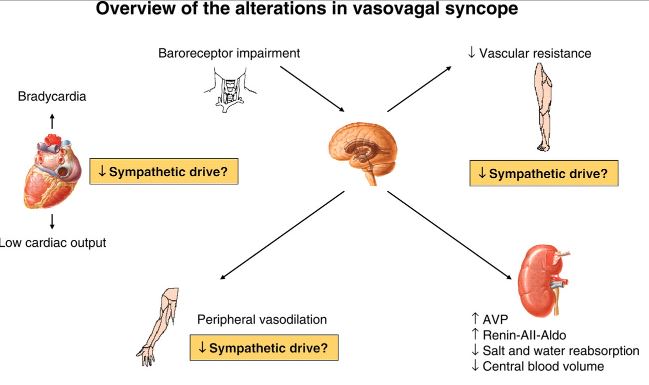
Pathophysiology of neurocardiogenic syncope
But the etiology of this condition is already described that neurogenic hypotension causes the syncope. Therefore, avoid the risk factors which can trigger the hypotension and syncope is followed.
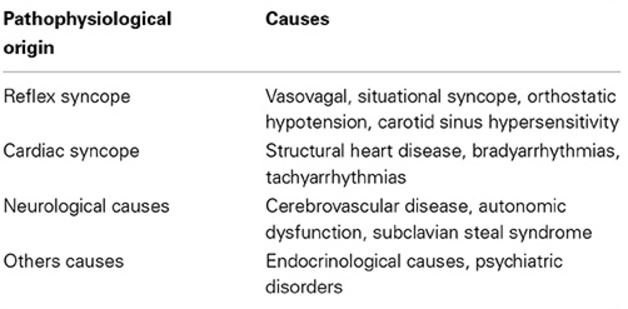
Different causes of types of syncope
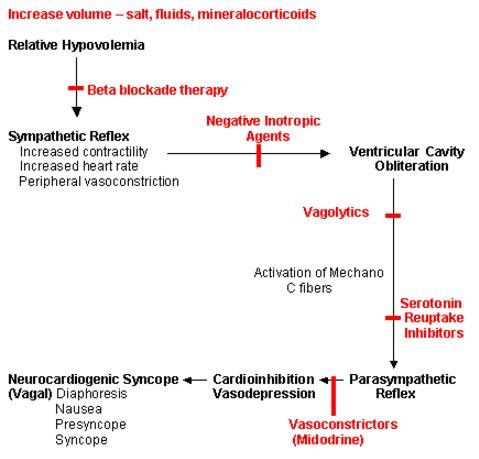
Risk factors
Following are the risk factors associated with neurocardiogenic syncope:
- Prolonged standing in a warm temperature, which makes people dehydrated and cause hypotension.
- extensive exercise
- Emotional stress
- Blood withdrawing
- Bowel movement after taking food , which starts the digestion and blood is circulated in the intestine.
- Alcohol intake
- Infection
- Low salt diet. Salt is harmful for hypertensive patient, but it is beneficial for hypotension. Salt helps to maintain the fluid volume in the blood vessels, so that pressure is maintained properly.
Treatment
The immediate care of neurocardiogenic syncope after an attack are
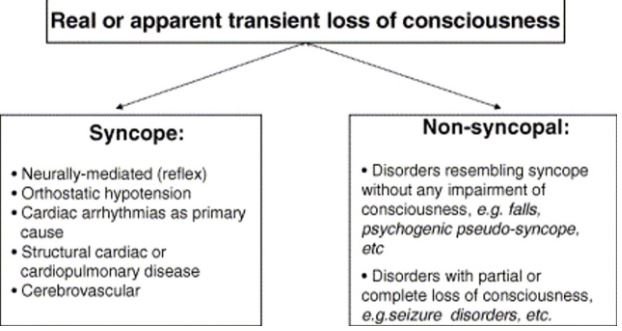
Transient Loss of consiousness (Syncopal, Nonsyncopal Causes)
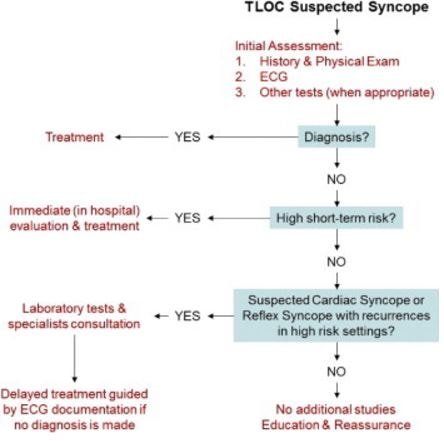
Assessment, Diagnosis and Management Protocol
- Patient should be in lying down position for at least 15 to 30minutes.
- Saline water or salty water intake helps to maintain the blood pressure.
- Patient should educate about risk factors and advice to take rest, if any of the symptoms occur.
- Some orthostatic training like standing against a wall for twice a day, may be beneficial.
The medical science advancement provides lots of treatment modalities for neurocardiogenic syncope. The suggested treatment depends on the age of the patient, tilt response, associated disease conditions and routine medications list.
General prescriptions
General prescriptions of the neurocardiogenic syncope contain following medications:
- Diuretics
- Centrally acting agents / or vasodilators including tricyclic antidepressants or MAO inhibitors.
But prolong use of these drugs may not be advisable, after a certain duration gradual withdrawn of drugs are recommended.
Pharmacologic Therapy
If the patient has chronic or repetitive neurocardiogenic syncope; then depending upon the patient specific factors, the following drugs doctors may prescribe:
- Steroidal drugs
- Beta blockers therapy
- Serotonin reuptake therapy
Cardiac Pacing
The cardiac pacing is another treatment option, though clinically it’s benefits in neurocardiogenic syncope remains in debate.
This therapy is particularly shows the beneficial effect for patients having bradycardial symptom. In addition, alone cardiac pacing may not be effectively treated neurocardiogenic syncope, additional medical therapy requires to obtain noticeable relief.
ICD9 Code
The billable medical code for neurocardiogenic syncope is ICD-9-CM 780.2, which can be mentioned to signify a diagnosis on a recompense claim.
Pictures
References
- Vasovagal syncope; Mayo Clinic Staff; Retrieve from: http://www.mayoclinic.org/diseases-conditions/vasovagal-syncope/symptoms-causes/dxc-20184778
- Neurocardiogenic Syncope; Comprehensive Cardiovascular Care Group; Retrieve from: http://www.cccgroup.info/neurosyn.asp
- Blair Grubb and Daniel J. Kosinski, (2001); Neurocardiogenic Syncope: When and How to Treat?; Retrieve from: https://www.uthsc.edu/cardiology/articles/neurocardiogenic%20syncope.pdf
- Syncope and collapse; Retrieve from: http://www.icd9data.com/2015/Volume1/780-799/780-789/780/780.2.htm
