Nuchal Translucency
Definition
Nuchal translucency abbreviated as NT is also called as nuchal translucency screening, nuchal fold test, prenatal genetic screening or a nuchal fold scan. This has been used as a sonographic prenatal screening test for the presence of Down’s syndrome in a fetus, especially among older women who are having a higher risk to this type of pregnancy.
It is best done during the 11th week and 14th week of the pregnancy or when the baby can attain a crown rump length (CRL) measurement ranging between 45 mm and 84 mm.
There are two available distinct NT measurements:
- Nuchal translucency which is taken at the earlier period of the pregnancy towards the end of the first trimester and early second trimester, with a lower threshold for an increased diameter
- Nuchal fold which is being measured towards the end portion of the second trimester
NT has been associated with Down syndrome, Turner syndrome, congenital heart disease, omphalocele, skeletal dysplasia, and congenital diaphragmatic herniation.
Indications of Nuchal Translucency
NT is indicated to be performed to all women with an increased risk of being pregnant with a fetus who might have Down syndrome or any other possible abnormalities in a more accurate manner, rather than basing solely on maternal age risk as a factor.
Procedure
Nuchal translucency is being measured utilizing a sagittal image going through the neck of the fetus. This is a specific tissue area located at the back of the neck an unborn baby.
An ultrasound procedure is used by the physician to measure the thickness of the nuchal fold.
The pregnant woman is instructed to have a full bladder in order to have the best ultrasound picture.
The correct techniques must be followed:
- Make sure that the vertebral column of the fetus is facing the bottom of the screen so that the viewed structures must be in the correct mid-sagittal position
- Magnification adjustment to allow only the head of the fetus and the upper portion of the thorax to be included in the image taken
- The head of the fetus should not be in an extended or flexed position
- Fetus should be floating freely from the uterine wall, allowing the amniotic fluid to be visually seen between the fetal back and the uterine wall
- Make sure that only the lucency is being measured with the use of the “+” calipers for measurement, taking into consideration that it is not the same with nuchal thickness
- The widest part of the area of translucency should be included in the measurement
Measurement
The NT normally grows in measurement as proportionate with the baby:
- NT less than 3.5 mm is normal when the baby’s CRL measures between 45mm and 84mm
- NT of 2.9mm is also within the normal range limit
- Babies with NT between 2.5mm and 3.55mm is considered completely fine
As NT increases, the risk of the baby to have Down’s syndrome also increases together with other types of chromosomal abnormalities:
- NT of 6mm with high risk for Down syndrome as well as other chromosomal and cardiac problems
Assessment Results
Results to be considered are as follows:
- CRL values between 45mm and 84mm is considered valid from 11.3 weeks to 13.6 weeks
- There is no septal deviation in the lucent region
- The nuchal thickness is directly related with the incidence of chromosomal problems and other congenital anomalies
- NT value that is lesser then 2.2mm to 2.8mm in thickness is not associated with an increased risk for chromosomal problems
- Nuchal translucency cannot be assessed when the fetal lie is unfavorable and the gestational age CRL is lesser than 45mm and greater then 84mm
Normal range
NT is specifically done at the right time of the pregnancy which is between the 11 weeks and 14 weeks period, or when the CRL measurement is between 45mm and 84mm respectively.
Normal results for Nuchal Translucency
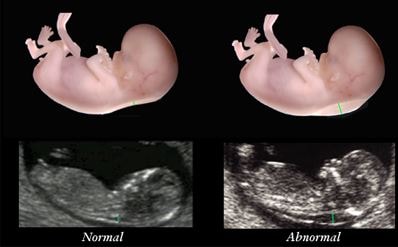
The normal amount of fluid found at the back of the fetal neck during an ultrasound procedure signifies that the baby is unlikely to develop Down syndrome or any other genetic problems.
- Normal measurement at 11 weeks age of gestation is up to 2mm
- Normal measurement at 13 weeks, 6 days age of gestation is up to 2.8mm
Meaning of Abnormal Results
The presence of more fluid at the back of the fetal neck means that the baby is at greater risk to develop Down syndrome.
Other procedures done when there are abnormal screening test results:
- Amniocentesis
- Chorionic villus sampling
- Fetal echocardiography
Treatment and Prognosis
As the second trimester is about to begin, the nuchal translucency region could either be:
- Regressing when the chromosome is normal, resulting to a normal outcome for the fetus also
- Evolving into cystic hygroma or nuchal edema
Differential diagnosis
Differential diagnosis is done in the presence of:
- An incorrect technique of the procedure
- Fetal neck skin thickening is a result of hydrops fetalis
- An amniotic membrane that is lying behind the fetal neck
- Presence of chorio-amniotic separation
References:
http://radiopaedia.org/articles/nuchal-translucency-1
http://www.babycentre.co.uk/a544491/nuchal-translucency-nt-scan
https://www.nlm.nih.gov/medlineplus/ency/article/007561.htm
Doubilet PM (2014). Ultrasound Evaluation of the First Trimester. Radiol. Clin. North Am. 52 (6): 1191-1199.
Simpson JL, Holzgreve W, Driscoll DA (2012). Genetic counseling and genetic screening. In: Gabbe SG, Niebyl JR, Simpson JL, et al, eds. Obstetrics: Normal and Problem Pregnancies. 6th ed. Philadelphia, PA: Elsevier Saunderschap 10.
Bromley B, Benacerraf B (2010). Chromosomal abnormalities. In: Rumack CM, Wilson SR, Charboneau JW, Levine D. Diagnostic Ultrasound. 4th ed. Philadelphia, PA: Elsevier Mosbychap 31.
