Vasa Previa
Vasa Previa Definition
Vasa previa is a rare type of condition that occurs when the blood vessels within the umbilical cord or placenta of the mother are being trapped in between the birth canal opening and the fetus. In this state, the fetus will be highly at risk of dying from hemorrhage due to a blood vessel ripping apart during the rupture of the fetal membranes, or at the time of labor and delivery.
The insufficient oxygen of the fetus is also considered a threat. Vasa previa might not be suspected by the physician not unless the fetal vessel rupture occurs. If the condition is discovered before labor, the baby will have a greater probability of surviving.
Symptoms of Vasa Previa
Vasa previa does not always show any signs and symptoms since the condition cannot be diagnosed until labor, or after a stillbirth. The blood of a baby is a darker red color caused by the low levels of oxygen. If the presence of a very dark burgundy blood is seen when the water breaks, this might be a sign of vasa previa.
Other possible symptoms may include:
- Painless bleeding of the vagina
- An abnormally low heart rate of the fetus
- Rupture of membranes
Causes
Vasa previa has not been studied well since it is a rare condition. A few experts believe that it can occur when the nutrients found at the lowest part of the placenta are not as rich compared to the ones that are situated at the top of the placenta. No one knows the exact cause of vasa previa, though there are some similarities by many patients.
Women who have this condition often experienced the following:
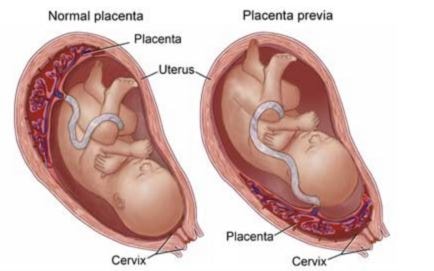
- Placenta previa wherein the placenta covers a part or the entire cervix during the last few months of pregnancy
- Pregnancies that are assisted by In vitro fetilization (IVF) in which the mature eggs are retrieved from the ovaries and fertilized by a sperm in a laboratory
- Previous pregnancies delivered through a Caesarean section
The reason of IVF being associated with vasa previa is not clear although several cases have been reported at approximately one in 300 for such pregnancies. Placenta previa which is also known as low-lying placenta, is related with vasa previa. These two conditions when combined, seem to produce an additional risk for the baby to be in a transverse position. This is due to the position of the placenta in the lower region of the uterus, preventing the fetus from presuming the correct head-down situation.
Diagnosis
A physician can pick up some signs of the vasa previa as early as the second trimester. The diagnosis can be done through:
- Prenatal ultrasonography which is an imaging test that can produce images of the baby developing in the womb. Vasa previa may already be suspected through this test.
- Transvaginal ultrasonography is a pelvic ultrasound used to examine the reproductive organs of a woman. Vasa previa is usually confirmed through this test.
- Doppler color flow mapping can be combined with transvaginal ultrasonography to help the physician detect the disease.
Treatment
Treatment options for vasa previa to decrease the damage that is possibly caused by ruptured blood vessels may include:
- Cesarean section birth might be recommended by the physician before labor and the medical team present during the delivery of the baby will most-likely prepare an immediate transfusion of blood for the baby in the occurrence of a rupture
- Ultrasound assessment is needed for evaluation of the cervix through transvaginal ultrasound at irregular intervals
- Admission may be necessary depending on certain circumstances of the mother
- Steroids might be prescribed in order to support for maturity of the lungs of the baby if in case it must be delivered prematurely by the mother. An amniotic fluid test could determine whether steroids are necessary.
Complications
Vasa previa can result to the following complications with the patient:
- Velamentous cord insertion where the umbilical cord of the fetus does not insert into the placenta but instead it inserts into the fetal membranes making it vulnerable to rupture.
- Succenturiate lobe which is a smaller lobe that is considered a risk for vasa previa development.
- Minor placenta previa in which the minor part of the placenta is low-lying.
References:
http://www.mountsinai.on.ca/care/placenta-clinic/complications/vasa-previa#riskfactors
http://www.medicinenet.com/script/main/art.asp?articlekey=5961
Hasegawa J, Farina A, Nakamura M, et-al (2010). Analysis of the ultrasonographic findings predictive of vasa previa. Prenat. Diagn. 30 (12-13): 1121-5.
Gagnon R, Morin L, Bly S, et-al (2009). Guidelines for the management of vasa previa. J Obstet Gynaecol Can. 31 (8): 748-60.
Yasmine Derbala, MD; Frantisek Grochal, MD; Philippe Jeanty, MD, PhD (2007). “Vasa previa”. Journal of Prenatal Medicine 2007 1 (1): 2–13.
