Vaginal Polyps
The vaginal lining is a suitable environment for the growth of vaginal polyps. The presence of these abnormal growth may occur often but they are usually benign [1].
Anatomy and Pathophysiology
The vagina is a muscular canal that connects the uterus to the outside. It has a soft and flexible lining that is responsible for lubrication and sensation during sexual intercourse. The vulva and the labia forms the entrance while the cervix form the interior end. Aside from its role in sexual intercourse, the vagina serves as the passageway for menstrual flow and the baby during a vaginal childbirth [1, 2].
Polyps are fleshy fingerlike growth that may develop in the vagina. These growths can be described as similar to skin tag in which the top part is connected to the body through a small stalk or stem. Majority of vaginal polyps are found to be benign and they are discovered during a routine pelvic examination. Although they may develop in any part of the body, polyps are typically found in the nasal passage, colon, cervix and vagina [3, 4].
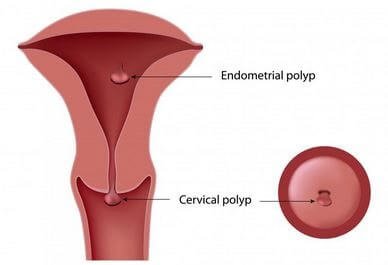
Figure 1 shows an example of a endometrial & cervical polyp.
ICD10
In the 2016 ICD-10-CM codes, the one that is used for the diagnosis of a vaginal polyp is N84.2. This code is for any benign polypoid growth or lesion that may arise from the walls of the vagina [5].
Causes of Vaginal Polyps
The exact cause of polyp development is not fully understood but studies have shown that vaginal polyps are more common during pregnancy. Polyps that have grown during this period do not require any treatment because they disappear after a few months after the baby has been delivered [6].
There are several studies that have shown that there are no links between the Human Papilloma Virus and the growth of vaginal polyp. This condition is also not transmitted through sexual contact [7].
Signs & Symptoms of Vaginal Polyps
Most women do not realize that they have a polyp in their vagina because of the absence of signs and symptoms. They is commonly just a single nodule in the vagina but there are instances that more than one polyp is present at once. The size of the polyp ranges from about 2mm to 5cm but there are cases where the vaginal polyp grow up to 20 cm in its size [7].
They may cause bleeding in the vagina after sexual intercourse. People who are in their menopause may experience vaginal discharge and heavy bleeding. This watery vaginal discharge can tur foul-smelling if the polyp has been twisted and infected [3].
Diagnosis of Vaginal Polyp
Health history and physical examination
Most vaginal polyps are discovered during a routine examination while there are others who sought consultation primarily due to the presence of vaginal bleeding and discharge. In the pelvic examination, a speculum will be inserted into the vagina to get a clear view of the whole area. Further tests may be requested by the physician once polyps are seen during the examination [3, 7].
Tissue biopsy
Although most of the vaginal polyps are found to be benign, a tissue biopsy must be performed to check the presence of cancerous cells. A sample of the tissue will be obtained by the physician during the pelvic examination and will be sent to the laboratory. This sample will be examined under a microscope in order to see the cellular make-up of the tissue [3, 7].
Treatment
Most vaginal polyps do not require treatment unless it has proven to be bothersome to the patient. If a patient for the polyp to be removed, she is advised that polyps may recur and there are currently no known methods to prevent its reoccurrence [4, 6, 7].
Removal
The removal of a vaginal polyp involves a simple surgical procedure that can be done in the outpatient department. After administering the anesthetic agent, the polyp is removed from its attachment from the vagina. Other removal options involves freezing the polyp or removing it through the use of a laser. These alternatives kill the polyp and a tissue biopsy can’t be performed on the vaginal polyp. Because of this, these methods are only advisable when the vaginal polyp is confirmed to be benign [6, 7].
After the procedure, the patient may experience some degree of pain or discomfort which can be managed through the use of oral pain medications. There are also those who may experience scant vaginal bleeding after the procedure. Patients should be advised that this may be expected but continuous bleeding should warrant a physician consult [6, 7].
References
- University of Iowa Hospitals and Clinics. (2015). Vaginal Cysts, Polyps, and Warts. Retrieved from University of Iowa Hospitals and Clinics: https://www.uihealthcare.org/vaginal-cysts-polyps-warts/
- (2015, October 22). Vagina. Retrieved from WebMD: http://www.webmd.com/women/picture-of-the-vagina?page=2
- Women’s Health Advice. (2015). Polyps. Retrieved from Women’s Health Advice: http://www.womens-health-advice.com/polyps/
- Wise Geek. (2015). What are Vaginal Polyps? Retrieved from Wise Geek: http://www.wisegeekhealth.com/what-are-vaginal-polyps.htm#comments
- ICD10 Data. (2015). Polyp of vagina. Retrieved from ICD10 Data: http://www.icd10data.com/ICD10CM/Codes/N00-N99/N80-N98/N84-/N84.2
- Innovate Us. (2015). What are the causes of Vaginal Polyps? Retrieved from Innovate Us: http://www.innovateus.net/innopedia/what-are-causes-vaginal-polyps
- Med, D. (2016, February 2). Fibroepithelial Polyp of Vagina. Retrieved from Dove Med: http://www.dovemed.com/diseases-conditions/fibroepithelial-polyp-vagina/
