Adenomyosis
What is adenomyosis?
Adenomyosis is a condition where the endometerium the inner lining of the uterus is shifted towards outer lining and uterus become thickening. The result of this condition is heavy menstrual flow with lower abdominal pain. The onset of this condition is common in case of middle aged women with history of pregnancy or any uterine surgical intervention. The triggering factor is mainly hormonal changes.
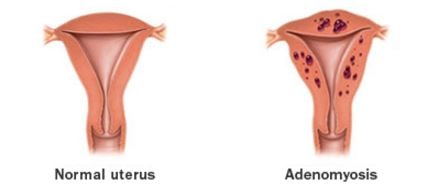
Often it has been seen that women have adenomyosis also develop endometriosis (the lining of the uterus is developed outside). It has been discussed that adenomyosis may interfere with fertility. This condition does not lead to life threatening for the patient, but it hampers the quality of life of the affected women.

Symptoms
The risk associated with sign and symptoms of the adenomyosis depends upon how much uterine muscle gets affected. This depends upon the degree of penetration and attachment of the uterine muscle. Some of the affected females are not having any symptoms, as in case of fibroids and endometriosis. The majority of the cases with enlargement of the uterus, the following symptoms are provided:
- Pain during menstrual cycle (Dysmenorrhea)
- Heavy bleeding during menstrual cycle (Hypermenorrhea)
- Duration of menstrual period increases
- Abdominal cramp
- Hefty clots
- Distend abdomen
- Lower back pain
- Chronic abdominal pain
- Discomfort and pain during sexual intercourse
- Nausea
- vomiting
Causes
The exact cause of adenomyosis is unknown. The suggested theoretical, hypothetical causes are:
Invasive tissue development: Some specialists suggest that invasive growth of endometrial cells at the uterine walls causes development of the adenomyosis. In cesarean section and other operations where the uterine incision is common has the probability to promote the invasive tissue growth on the wall of the uterus.
Fetus developmental phase: Some experts believe that the endometrial tissue deposition can be obtained at the fetus development phase inside the uterus. This unwanted tissue development can lead to adenomyosis.
Stem cell origins: Recent assumption is that stem cells originated from bone marrow may raid the uterine muscle and leads to adenomyosis.
Despites the consequences of an adenomyosis development, the estrogen present in the blood circulation can promote the development of the adenomyosis. After menopause, due to the reduction of the estrogen level in a woman’s body causes adenomyosis rid of.
Diagnosis
If the affected woman does not have any associated problem with adenomyosis, then the diagnosis can be conducted. For confirmatory test, diagnosis can only possible after conduction of hysterectomy.
Physical examination
Initial diagnosis is conducted by physical examination and a usual finding during physical examination is the mass or the elevation of the uterine wall or tenderness at the uterine wall.
The imaginary tools are used to diagnose the symptoms menorrhagia and dysmenorrheal and these symptoms are associated with adenomyosis.
Pelvic Ultrasonography
In case of adenomyosis, ultrasonographic interpretation is not well significant. The usual findings after pelvic ultrasonography are as follows:
- The uterus is normal in appearance
- At the posterior wall, typical focal or diffuse thickening is noticeable
- Thickness of the endometrial layer is greater than 12mm, this observation is not usual. It is observable when transitional zone is visualized.
- Specific sign can be obtained if subendometrial echogenic nodules are observed.
- The findings of tiny myometrial cysts or sub endometrial cysts are also specific sign.
Specifically for transvaginal ultrasound, following are the specific findings:
- Uterine enlargement
- Increase thickening of the uterine wall
- Linear striations at the endometrial layer.
- Transition zone thickness increases with 12mm or greater.
If the definite result is not obtained from adenomyosis, then doctor may recommend MRI can provide better confirmatory interpretation.
Management
Treatment management plan can be depends upon the severity of the symptoms and also age of the patient:
Anti-inflammatory drugs
In case of a patient nearly at the age of menopause, then doctors usually prescribed anti-inflammatory drugs during the dates of the menstruation cycle to control the pain. Anti-inflammatory medications can help for heavy flow.
Hormonal therapy
Hormonal therapy mainly estrogen-progestin regulating therapy is helpful for this condition. Doctors mainly prescribe this medication available as contraceptive pills or intra uterine device to control pain. This treatment approach can be helpful for controlling bleeding.
Surgical management
Hysterectomy
One of the traditional surgical interventions is hysterectomy. Though this is not well accepted, as in hysterectomy, complete removal of uterus is conducted and it also creates lots of hormonal imbalance. But in case of severe pain, long way to reach in menopause and heavy flow, which affect patient’s quality of life, then doctor may recommend hysterectomy.
Other than hysterectomy, the two novel surgical interventions are
- Uterine artery embolization and
- MRI-guided focused ultrasound surgery
Uterine artery embolization
For establishing this treatment, different clinical trial is conducted. This is a not comes under the major surgical intervention, but by conducting a minimal invasion, insertion of small particles able to obstruct the arteries which restrict the blood flow in adenomyosis.
For inserting the small particles in to the blood vessels, a tiny tube is introduced through the cervix and reached to the vagina. Blockage of blood flow causes shrinkage of adenomyosis . This is a widely accepted medical technique for shrinkage of fibroids.
MRI-guided Focused Ultrasound Surgery
The clinical data provide the evidence that lesions cause by adenomyosis can be adequately ablated seal to the endometrium or serosal surface. This evidence provides the information that MRI-guided Focused Ultrasound surgery is a novel, safe and successful method for the ablation of adenomyotic tissue.
References
- http://www.jultrasoundmed.org/content/31/5/805.full.pdf
- http://www.medscape.com/viewarticle/703820_11
- http://www.mayoclinic.org/diseases-conditions/adenomyosis/basics/treatment/con-20024740
- http://www.webmd.com/women/guide/adenomyosis-symptoms-causes-treatments?page=2
- Diagnosing and Detecting Adenomyosis, The Emotional and Psychological Effects of Adenomyosis, How can Female Alternative Surgery help you??? at http://www.alternativesurgery.com/education/adenomyosis/
- Adenomyosis: Risk Factors, Symptoms & Diagnosis at http://www.healthline.com/health/adenomyosis#Overview1
